25 March 2022 – Author: Petra Teunissen. This article was published in the professional journal VoetVak+ for medical and cosmetic foot care.
Infection is one of the most common complications of poorly healing wounds. Many pedicurists see nasty ulcers on the feet of diabetic patients. Antibacterial treatments are indispensable for these infected wounds. A relatively new method works with cold plasma. Koen Lim, medical officer of Plasmacure, talks about this innovative ‘lightning plaster’ for the treatment of chronic open wounds.

Koen Lim, Plasmacure medical officer, with PLASOMA.
In people with poor blood circulation due to vascular disease or in diabetes patients, wound healing is often severely disrupted. If they have a small wound, this can lead to a chronic open wound. This mainly happens on the lower legs and feet, because they are far from the heart and the blood circulation there is less good. Chronic wounds are an underestimated problem. In the Netherlands, there are about half a million people with chronic wounds and about twenty-five percent of them have a wound that hardly ever closes. The wounds have a lot of impact on a person’s life and their environment. Frequent wound care takes a lot of time and hinders the patient’s social life. The patient cannot shower or swim comfortably. The wounds sometimes have a smell and people are ashamed of them. Chronic wound care is expensive. It is estimated that the Netherlands spends about two billion a year on this care. Due to the increase in obesity, diabetes and an aging population, the number of people with chronic wounds is growing by 5 to 6 percent per year. Moreover, clinical wound care is fragmented across the disciplines of internal medicine (diabetes), vascular surgery, rehabilitation and dermatology.
GAS CHARGED WITH ENERGY
The Dutch company Plasmacure has developed a treatment system based on cold plasma, PLASOMA. Koen Lim, doctor and business administrator, explains: “Plasma is the so-called fourth phase of a substance, after solid, liquid and gas. The sun, lightning and the northern lights are all examples of plasma, and they are created by charging a gas with energy. This ionizes the gas and it creates a mixture of reactive compounds, such as ozone, nitrogen oxides and hydrogen peroxide. Plasma is used to kill bacteria and viruses because they cannot create a resistance to it.
Koen Lim continues: “Plasma medicine is a new field of application. Normally plasma is very hot, but certain techniques are used to make cold plasma. Cold plasma has nothing to do with blood plasma. In cold plasma, the temperature does not rise far above the body temperature. In medicine, various fields of application are being investigated, for example cancer, bone fractures and dermatology (acne). At Plasmacure, we focus on wound care. More than ten years ago, we started developing a method to heal a chronic open wound with cold plasma. Cold plasma has the following mechanisms*:
• Cold plasma inactivates (multidrug resistant / antibiotic resistant) bacteria, viruses, fungi and yeasts. After a few seconds of cold plasma, only 1 in 100,000 MRSA bacteria, the infamous “hospital bacteria” survives. Staphylococcus aureus, which is often found in open wounds, also gets killed. The plasma also inactivates the bacteria that ‘hide’ in the biofilm on the wound. It is important that the plasma penetrates the biofilms, because such a slippery layer of micro-organisms often prevents wound healing.
• Cold plasma stimulates cell migration and cell proliferation. Research has shown that after exposure of 1 and 3 minutes, the cells that repair the epidermis, such as fibroblasts and keratinocytes, became more active. They produce growth factors to grow healthy skin from the wound edges.
• Cold plasma stimulates microcirculation. Within 10 minutes of treatment, the hemoglobin level and oxygen saturation increased significantly. Cold plasma not only affects blood flow at the surface, but up to a depth of 8 mm. The extra oxygen exites the ‘sleeping’ cells.
In summary: cold plasma can turn a chronic wound that doesn’t show any signs of improvement into a wound that starts getting better.”
“More than ten years ago, we started developing a method for healing a chronic open wound with cold plasma.”

Diabetes podiatrist Ingrid Ruys is conducting a study with PLASOMA at the Máxima Medical Center in Veldhoven.
THE DEVICE
PLASOMA uses a flexible ‘pad’ that is fixed on the wound. The pad has a cold plasma area with a diameter of 3 cm, suitable for most diabetic foot ulcers and open leg wounds. PLASOMA cold plasma pulser sends an electrical current to the pad to create the cold plasma between the pad and the wound. Then the treatment, which lasts 2 minutes, begins: three times a 20-second round of plasma followed by a 20-second break to allow the substances to take effect. In total, the patient receives 1 minute of cold plasma. After treatment, the pad is removed and discarded. The treatment is well tolerated, the patient sometimes feels a slight tingling.
CASE STUDIES AND CLINICAL STUDIES
Koen Lim: “The clinical safety study conducted in Amsterdam UMC showed that PLASOMA indeed kills bacteria in chronic wounds in a safe way. Case studies are being conducted to gather more data. The first 20 treated wounds from these case studies were on average 65 weeks old and treated for an average of 8 weeks. 60 percent of wounds are closed/healed within an average of 7 weeks and 13 treatments. We are very happy with these great results. The treatment normally takes place once or twice a week, always in addition to normal wound care, sometimes in combination with total contact casting. As a practitioner, it will be possible to see if it is working or not after a few weeks. If it works, you finish the treatment and if not, you stop after a month. Motivating the patient to adhere to the precepts remains important. Offloading (reducing weight and friction) remains necessary in order not to hinder the healing process.”
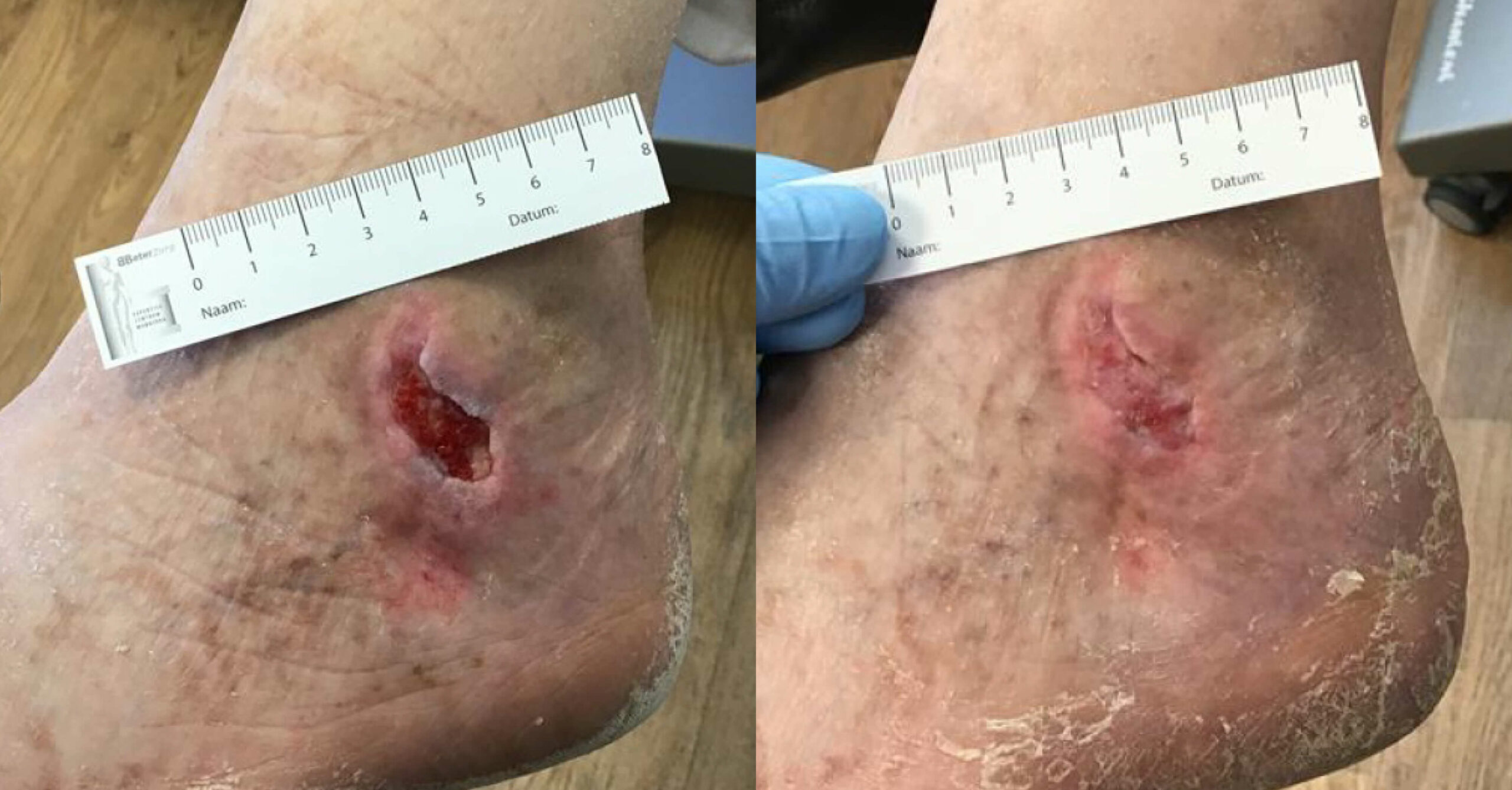
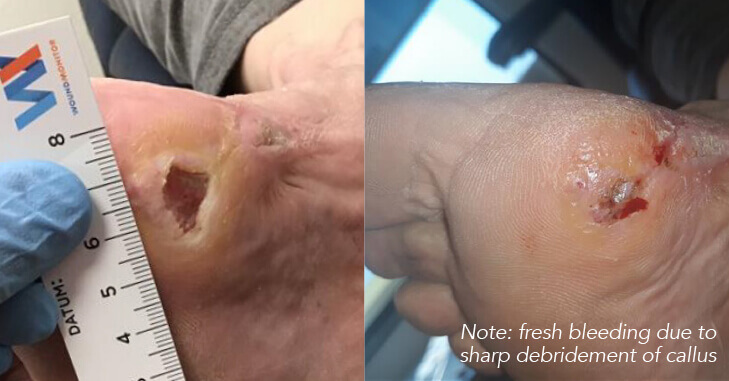
Results from the case studies.
“We focus partly on severe chronic wounds. The case studies included many diabetes patients, but also people who have had a skin graft. The device is portable. We are now working on making this technique suitable for home treatment. This is because 80 percent of patients with chronic wounds live at home, and it is mainly people over the age of 70 who are less mobile. Home treatment not only offers them comfort, but health care insurers also want people to visit the hospital less often. In addition, doctors can see their patients less often than healthcare professionals in secondary or tertiary care facilities. For the time being, the treatment must be carried out by someone with good training and experience in wound care. Careful debridement is also very important (removal of necrotic (dead) tissue, fibrinous deposits and other wound debris). The cold plasma treatment follows the cleaning of the wound. Perhaps in the future, if more accessible methods for debridement are available, medical pedicurists will also be able to perform the cold plasma treatment in collaboration with or on the instructions of a podiatrist or wound nurse.”
THE DIABETES PODOTHERAPIST
Diabetes podiatrist Ingrid Ruys works in the multidisciplinary foot team in the Internal Medicine department at the Máxima Medical Center in Veldhoven. She is participating in a clinical study with PLASOMA cold plasma that also includes a control group that receives wound treatment without cold plasma. Since the spring of 2021, Ingrid has treated about thirteen patients. She sees the patients weekly until the wound is closed, for a maximum of twelve weeks in a row. All patients receive a follow-up trajectory.
“Treatment normally takes place once or twice a week, always in addition to normal wound care.”
The results are variable, says Ingrid: “In some wounds you see promising improvement, in others almost nothing. But the group researched is still too small to make definitive statements about this. What I especially like is that I can see the patients every week. Whether they are in the treatment group or control group. Then you can see the changes better. To the detriment or to the advantage.” Ingrid has seen many ‘serious cases’ in her consulting room in Máxima Medical Center for 22 years: “I have good contact with the approximately 120 medical pedicures with whom I have agreements. If they see something strange, they contact me via the Silo communication system. That network works like a train, which is really nice. I give them my trust and radiate that to my colleagues. Then I point out to our team that the patient’s pedicurist reports the wound and does not cause it. This way the pedicurist gets more credits. But I am hesitant to transfer this wound care to pedicures. A wound on a diabetic foot can be so dangerous if you lack symptoms. Here I can have extra examinations, wound cultures and X-rays. I actually probe all wounds, because I want to know how deep the wound is. Do I have bone contact or not? And I always have colleagues nearby for advice and consultation, such as internists, rehabilitation doctors or vascular surgeons. As soon as the wound has calmed down, the patient can of course return to the medical pedicure.”
*see whitepaper: Stimulating wound healing using cold plasma


